Cervical Cancer Screening
Charles Savona-Ventura MD DScMed FRCOG AccrCOG MRCPI
Professor of Obstetrics & Gynaecology
Faculty of Medicine & Surgery, University of Malta
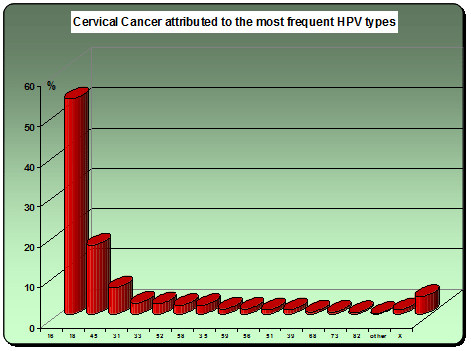
The first realization that cervical cancer was a sexually transmitted disease was originally made in the mid-nineteenth century by the Italian chief physician of a Verona hospital and an instructor at the University of Padua, Domenico Antonio Rigoni-Stern. In his presentation to the Surgeons’ Subgroup of the IV Congress of the Italian Scientists delivered on 23 September 1842, Rigori-Stern reported that in his review of the death registries of the town and suburbs of Verona over a period covering 80 years [1760 – 1839], cancer of the cervix of the uterus was noted to be rare in nuns and unmarried women, but widespread in housewives, suggesting a sexual link with the malignancy. As usually happens with a landmark observation, Rigoni-Stern’s observations were completely ignored for the next hundred years. Interest in the aetiology and epidemiology of cervical cancer was revived during the 1940s, when a number of studies confirmed Rigoni-Stern’s findings and the general consensus accepted that cervical neoplasia had the characteristics of a venereal transmitted disease. The true causative agent was however only identified in 1976. This cancer appears to be caused by several types of the human papillomavirus (HPV), particularly the subtypes HPV 16, 18, 31 and 45; though a number of other subtypes account for other occasional cases. This virus is introduced into the genital tract during sexual but not necessarily penetrative intercourse; it then resides there causing gradual changes in the cervical epithelium that progress from early cellular changes, to epithelial thickening, to precancerous states and on to full-blown cancer.1
Cervical cancer in the world is the fifth most deadly cancer in women; affecting about 1 per 123 women per year and killing about 9 women per 100,000 per year. It is estimated that there are at any one time about 473,000 women affected by the cervical malignancy; more than half will succumb to the disease. The incidence rates of cervical cancer in various populations and communities vary in accordance to the sexual practices of that community, being higher in more promiscuous societies. The incidence of cervical cancer reported in Europe and the Eastern Mediterranean lands varies from the high 27.3 per 100,000 women in Serbia & Montenegro to the low 2 per 100,000 women in the Syrian Arab Republic. The rate in the Maltese Islands was reported at 4.8 per 100,000 women, placing the Maltese population in the ninth place of the European-Middle East low risk chart (Figure 1). It is telling that except for Finland, the eight countries who reported lower rates include populations from the Syrian Arab Republic, Iraq, Qatar, Jordan, Israel, Turkey and Saudi Arabia.2
|
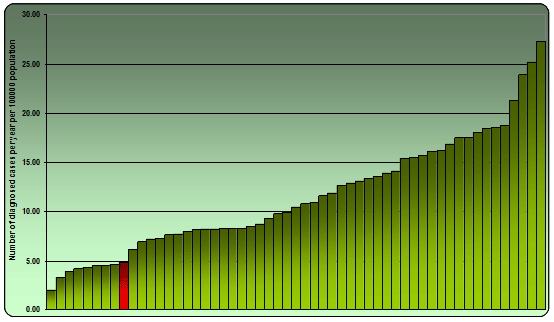
Incidence Rates of Cervical cancer in the European-Middle East Region: 2002
Source: Globocan 2002
The advent of the sexual revolution in Europe experienced during the “swinging sixties” – delayed in Malta to the 1980s because of the previously strong Roman Catholic moral influence – should have led to an increase in incidence rates in most sexually progressive communities. This rise in incidence rates has been observed but has not been as dramatic as one would have expected because of the contemporary introduction of effective screening programmes. Cervical cancer and precancerous lesions are relatively easy to look out for by visualizing the cervix and sampling the cells from the organ. The national service of population screening for cervical carcinoma was introduced in the government hospitals in 1977 and expanded to the specialist community health centres or polyclinics in 1982. This was complimented by the service offered in the private health sector. The programme however was and remains an opportunistic one whereby it is left to the individual woman to seek screening. Many women fail to get themselves screened or do not screen themselves regularly. The National Health Information Study conducted in 2002 among a randomized sample of the Maltese population has shown that only 45.1% of women interviewed reported having a smear test in the three years prior to the survey; 41.1% reported never having a smear test done and 13.8% reported that the most recent smear was performed more than three years before.3 The last two decades in Malta have seen a fall in the incidence of cervical cancer but a significant rise in the number of premalignant cervical lesion and HPV-infections. This observation suggests that, in spite of the rather opportunistic screening programme in place on the Islands, the large majority of potentially malignant cases are being identified and treated early before they become fully malignant.
The cervical smear sampling technique was invented by Georgios Papanokolaou in 1928 originally intended to detect cyclical hormonal changes in the vaginal cells and later developed into a cancer screening test in 1941. The test has changed very little since its invention; though the last decade has seen the development of liquid-based cell thin-layer technology which makes interpretation of the smear less susceptible to false results. The test remains an effective, widely used method for early detection of cervical cancer and pre-cancer. There is no definite screening protocol, since this varies from one country to another depending on the health services facilities available in each individual country. Countries with a comprehensive health service, like the United Kingdom, propose a screening protocol based on a balance of clinical risks and cost concerns with the aim of covering a wide section of the population with the least cost. Other countries, often those whose national health service is not comprehensive, recommend more frequent screening. The American guidelines mainly base the recommendations on clinical risk status rather than on cost concerns.
Women with extremely low risk status – virginal women, after hysterectomy with removal of the cervix, or those aged over 65 years who have had at least 10 normal smears – can opt out from performing regular cervical smears. These extremely low risk women however can still develop different relatively rare forms of cervical cancer which have no relationship to sexual activity. Those considered to be low risk women – women with less than three sexual lifetime partners, no history of sexually transmitted disease, and onset of sexual activity after 20 years of age – are advised to commence cervical cancer screening at least three years after the first sexual experience, followed up by annual smears until the age of 30 years, and subsequently 2-3 yearly until the age of 65 years. Those women who are known to be at high risk of developing cervical cancer – women with more than three lifetime sexual partners, an early sexual experience, a history of some form of sexually transmitted disease, and a history of an abnormal cervical smear in the past – should opt for an initial twice yearly screening followed by annual testing until there are three consecutive normal results after which they should opt for 2-3 yearly screening until the age of 65 years, provided subsequent smears remain normal.
Cervical screening alone cannot be considered sufficient for diagnosis since false positive results can occur with the crude simple screening test. An abnormal cervical smear result is usually followed by a more detailed examination using a colposcope. This instrument is basically a ‘magnifying glass’ that allows the clinician to examine the cervix under magnification to identify and biopsy any sites which appear possibly abnormal. A colposcopic service enabling the better investigation and management of premalignant lesions was first introduced in Malta in 1987. The biopsy can then give a more definite diagnosis upon which a clinical decision regarding management can be made. Depending on the severity of the condition, the management can range from regular follow-ups to local destruction of the lesion, to excision of the cervix to an extensive hysterectomy.
All these facilities have helped reduce the mortality of cervical cancer in the Maltese Islands from the level of 4.8 per 100,000 women in the early 1960s to 3 in the early 2000’s. This reduction has occurred in spite of the increase in sexual activity which has occurred in the last decades.4 A recent survey has shown that only 20% of Maltese individuals reported having one sexual partner, 23% reported having had more than 10 partners. The first sexual encounter on average occurs at about 19 years of age; however 22% of girls and 13% of boys had their first sexual encounter by 15 years of age.5
The fight against this destructive disease has however been limited in the sense that attempts have been done to identify and treat premalignant conditions early. The screening methods in place therefore help reduce the incidence and hence mortality of cervical cancer; but they do not help reduce the rising incidence of cervical premalignant conditions brought on by an increasing promiscuous lifestyle. They do not offer any prevention against the infection. The breakthrough in prevention has come in recent years by the introduction of specific vaccines to protect against the two subtypes of the HPV most responsible for the development of cervical cancer. Two vaccines have been introduced locally by different companies. Both protect against subtypes HPV 16 and 18 that account for over 70% of cervical cancer cases. They also seem to have crossover cover against other HPV subtypes. Obviously, protective cover is only effective provided the woman has not been previously infected. Hence it is recommended that ideally the vaccine is administered to females before they become sexually active starting by vaccinating children aged 10 years. Because of the rarer forms of HPV subtypes that cause cervical lesions and which are not covered by the vaccine, the administration of the vaccine does not exclude the need for continuing with a scheme of cervical screening. One would hope that the Maltese health authorities will be bold enough to emulate their counterparts in other European countries and introduce the vaccine in the vaccination schedule currently in force. The economic costs of vaccination far outplay the economic, psychological and physical costs of treating cervical premalignant and malignant lesions.
References
1. Kaufman RH, Adam E. Herpes simplex virus and human papilloma virus in the development of cervical carcinoma. Clinical Obstetrics and Gynecology 1986; 29:678-92.
2. Ferlay J, Bray F, Pisani P, Parkin DM. GLOBOCAN 2002. Cancer Incidence, Mortality and Prevalence Worldwide. IARC CancerBase No. 5, version 2.0, IARCPress, Lyon, 2004. Accessible from: http://www-dep.iarc.fr/
3. Department of Health Information. The First National Health Interview Survey, – Summary Statistics. FHI, Malta, 2003 [downloaded from http://www.sahha.gov.mt].
4. Buttigieg GG, Savona-Ventura C, Vella K, Cassar O. Cervical Carcinoma in the Maltese population. International Journal of Risk and Safety in Medicine 2008; 20(4):223-30.
5. Mifsud M, Buttigieg GG, Savona-Ventura C, Delicata S. Reproductive health in Malta. The European Journal of Contraception and Reproductive Health Care 2009; in press.

