Imaging Thyroid Cancer
Pierre Vassallo
there are four main types of thyroid cancer: papillary, follicular, medullary and anaplastic types. Papillary and follicular cancers are well-differentiated cancers that originate from the thyroid follicle. Tey are the more common types of thyroid cancer,
accounting for 80% and 10% of cases, respectively.1 Most clinically and ultrasound-detected thyroid nodules are benign, many representing purely cystic lesions known as colloid cysts. Solid or partly solid nodules however, should be further
investigated since approximately one in four will be malignant. Although differentiated thyroid cancers are generally slow growing, lymph node metastases are present in 30-80% of cases at the time of frst diagnosis.2 Te outcome of treatment is good
with a 98% 5-year survival,3 but these results depend on proper surgical treatment.
Te presence of lymph node metastases is the most common cause of thyroid cancer recurrence. Since most recurrences occur within the frst fve post-operative years, they may likely result from inadequate detection and resection at the time of initial
management.4 Physical examination has shown poor accuracy in detection of lymph node metastases. Accurate staging of thyroid cancer depends on meticulous ultrasound evaluation and detailed reporting, which are crucial for accurate surgical planning.
NECK ANATOMY
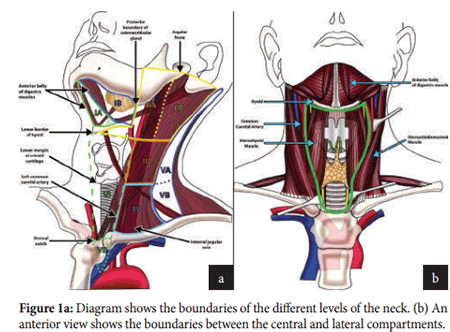
To ensure a clear communication between the radiologist and the surgeon, we share a common nomenclature for indicating the location of abnormal ultrasound fndings. Te neck is divided into seven levels as shown in fgure 1. Te aim is to standardise terminology related to surgical dissections for head and neck cancer. Level VI is considered the central compartment and it contains the thyroid gland; it is bordered by the hyoid bone superiorly, the carotid arteries and sternocleidomastoid muscles laterally and the sternal notch inferiorly. Tis is the most common site for lymph node metastases and cancer recurrence.
Te lateral compartment is mainly composed of levels II-VI with levels I and VI being less frequently involved; metastatic disease in this compartment is associated with a worse prognosis.
SURGICAL TECHNIQUE
There are multiple surgical procedures that can be performed to treat thyroid cancer; the aim however is to excise all locations of disease, as surgical excision is the most effective mode of therapy. All solid or partly solid nodules require biopsy. Tis consists
of a fne needle aspiration (FNA) that is performed under ultrasound guidance. Biopsy-confrmed malignant nodules are excised and the surgical approach depends on the location and number of malignant nodules found.
Unilateral nodules ≤1cm in diameter are treated with thyroid lobectomy, while nodules >4cm in diameter require a total thyroidectomy. For solitary nodules measuring 1-4cm in diameter with no lymph node metastases, a thyroid lobectomy is
usually performed although some surgeons prefer to perform a total thyroidectomy. For bilateral malignant nodules and in the presence of regional or distant metastases a total thyroidectomy is required along with resection of any lymph node metastases.
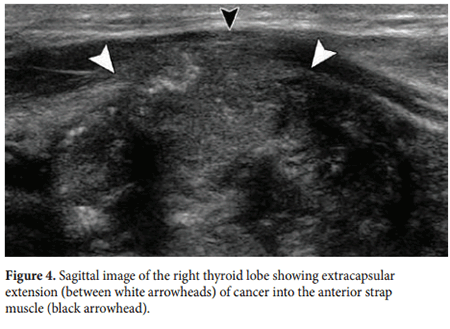
In the case of extracapsular invasion by thyroid cancer into adjacent structures (e.g. strap muscles of the neck), the involved structures must also be excised.
The risks of total thyroidectomy include bilateral recurrent laryngeal nerve paralysis and permanent hypocalcaemia due to parathyroid gland damage. Proper lymph node dissection is key for reducing the risk of recurrence. The nomenclature used for lymph node
dissection depends on the extent of dissection performed. A radical lymph node dissection involves resection of level I-V lymph nodes, the sternocleidomastoid muscle, the jugular vein and the superficial accessory nerve, while an extended radical dissection includes excision of any further involved structures. If any structures are retained, such as the jugular vein, the procedure is called a modified (or selective) radical dissection.
The term central compartment neck dissection refers to removal of all involved structures and lymph nodes in level V, while a lateral compartment neck dissection includes dissection of involved structures and lymph nodes in levels II-V.
ULTRASOUND TECHNIQUE
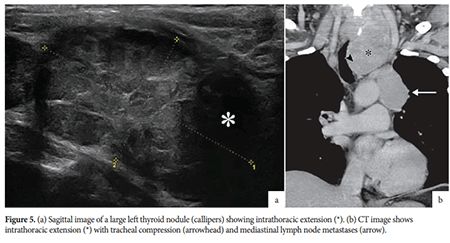
During the ultrasound scan, the whole thyroid gland and all potential areas of metastatic disease must be evaluated. All abnormalities must be described in detail based on their morphology and size, and their locations mapped according to the levels described above. Accurate description of the morphology and location of all foci of disease is crucial for guiding completed excision to reduce the risk of recurrence. Tere are some features that increase the level of suspicion when assessing thyroid nodules. A purely cystic lesion with a thin wall and no solid component is benign and does not require any follow-up. All solid or partly solid nodules with suspicious features and measuring ≥1cm in diameter require FNA evaluation. Ultrasound must also identify bilateral location of nodules, extracapsular extension (e.g. strap muscles) and retrosternal extension. Retrosternal extension should be further evaluated with computed tomography (CT) to detect extent of direct extension and the presence of mediastinal lymph node metastases.
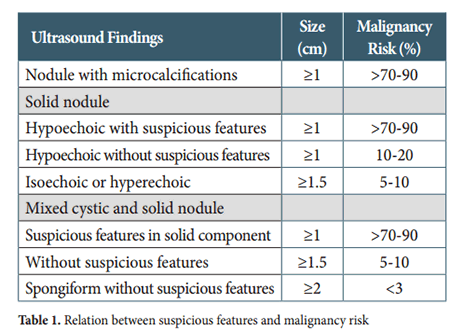
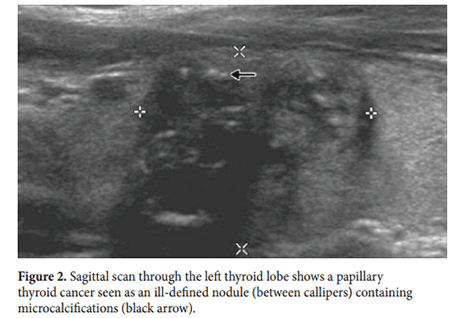
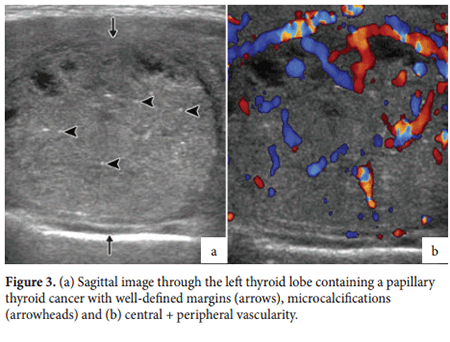
Suspicious features in a thyroid nodule include a size ≥1cm, solid components, a shape that is taller than wide, irregular or lobulated margins, microcalcifcations, interrupted rim calcifcations, extra-thyroid extension into adjacent structures and presence both peripheral and central vascularity. Te presence of microcalcifcations is highly suggestive of malignant disease having a sensitivity of 89%, a specifcity of 95% and an accuracy of 94% (Figure 2). Other features such as size, shape, irregularity of margins, extra-thyroid extension (Figure 3 and 4) and central vascularity are all important when planning FNA procedures. Table 1 shows how suspicious features relate to the risk of malignancy as taken from the American Tyroid Association consensus report of 2015.5 Detailed evaluation of lymph nodes at all neck levels is required.
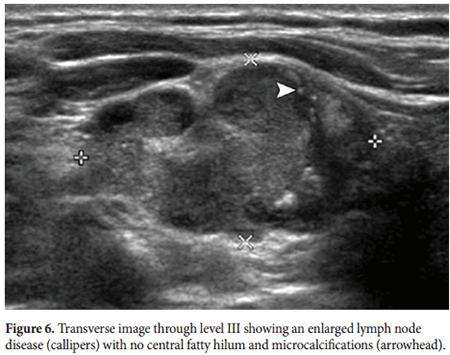
Size is not a reliable criterion for excluding metastatic disease; normal cut-off size is <0.8cm in level II and <0.5cm in levels III-VII. Microcalcifcations and cystic degeneration within a lymph node are strongly suggestive of metastatic disease with a high degree of accuracy (Figure 5). Increased peripheral vascularity is also indicative of metastatic disease. Additional suspicious features include echogenicity greater than adjacent muscle, a rounded shape (long-to-short-axis ratio <2) and loss of the central fatty hilum.
During thyroid surgery, the central compartment is always exposed, while the lateral compartment is only exposed if FNA-proven lymph node metastases are present. Tus, accurate pre-operative mapping of all ultrasound detected sites of disease is required to guide the surgical approach. post-operatIve ultrasounD evaluatIon In the immediate post-operative period, numerous nodules may be seen in the thyroid bed that are benign. In fact, 90% of nodules measuring up to 11mm in diameter seen in the immediate post-operative period are benign.6 Post-operative assessment with ultrasound should not be performed earlier than three months afer surgery.
Residual thyroid tissue may be noted on post-operative scans as iso- or hyperechoic nodules. Hypoechoic nodules should raise suspicion for malignant disease. An increasing serum thyroglobulin level (repeated 6-12 months afer surgery) is also suggestive of recurrence.
CONCLUSION
Complete surgical excision is the most effective treatment for thyroid cancer. Detailed analysis and mapping of all sites of disease and clear communication with the surgeon are crucial for preventing recurrence.