Carpometacarpal Osteoarthritis on the Thumb
Mr Alistair Pace
INTRODUCTION
Osteoarthritis of the trapeziometacarpal joint is the second most common site of degenerative joint disease in the hand and mostly affects postmenopausal women and manual workers. The reported radiographic prevalence of the condition is 7% in males and 15% in females. Studies reveal that 33% of women over 40 years of age will have some Xray changes. To achieve a high degree of prehensile and manipulative function this highly mobile joint is constrained by both the biconcave saddle morphology of the trapezium and the ligamentous constraints. It is theorized that attenuation of the anterior oblique ligament or beak ligament leads to instability, subluxation and eventually arthritis of the CMC (carpometacarpal) joint. The condition can cause pain, weakness, deformity and loss of function of the thumb and can be very debilitating.1
SYMPTOMS AND SIGNS
The symptoms vary in severity and usually progress over time. Patients usually present with swelling at the base of the thumb as well as aching, discomfort and tenderness. They report a limited range of movement and stiffness as well as loss of strength. Typically they complain of pain with rotatory movements of the thumb in particular opening jam jars or taps. On examination there may be squaring of the base of the thumb due to subluxation of the CMC joint of the thumb particularly in advanced cases. There may also be wasting of the thenar eminence particularly the APB (abductor pollicis brevis) due to stiffness (Figure 1). Furthermore there may be compensatory hyperextension of the MCP (metacarpophalangeal) joint of the thumb. Movements of the thumb are usually limited and associated with crepitus. There may be a positive axial loading grinding test. If there is associated arthritis in the STT (scapho-trapezio-trapezoid) joint then there will be pain on radial deviation of the wrist. In 50% of cases there may be concomitant carpal tunnel syndrome.
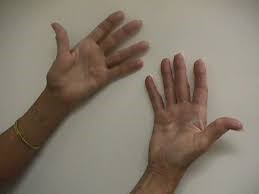
Figure 1: Clinical signs of base-of-thumb arthritis
RADIOLOGY
The optimal view requires the Xray beam to be centred on the trapezium and metacarpal with the thumb flat on the cassette and thumb hyperpronated. The conditions present with
narrowing of the CMC joint of the thumb, osteophytes, sclerosis and subluxation (Figure 2)
The clinical signs do not correlate with radiographic findings. In fact whilst symptomatic hand osteoarthritis affects approximately 25% of adult subjects, radiographic changes can be found in up to two thirds of females and half of males older than 55 years of age. The most widely used classification system for the radiographic staging of thumb CMC osteoarthritis is the Eaton and Littler classification ranging from mild (stages 1 and 2) to severe (stage 4) disease associated with pan-trapezial arthritis.1
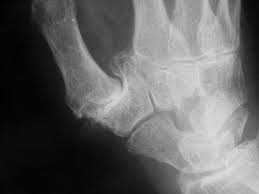
Figure 2: Radiographic feature of base-of-thumb arthritis
TREATMENT
In the early stages the condition can be satisfactorily treated with NSAIDS, thumb strengthening exercises of the thenar eminence, modification of activities and splinting or bracing of the thumb e.g. a thumb wrap. A variety of injections including steroid injections, hyaluronic acid intra-articular injections and PRP (platelet-rich plasma) injections have been trailed. A prospective randomized double blind controlled clinical trial comparing PRP and corticosteroid injections confirmed that corticosteroids offer short term relief of symptoms but PrP might achieve a lasting effect of up to 12 months in the treatment of early to moderate TMJ (temporomandibular) arthritis.2 Moreover hyaluronic acid injections show no difference for the relief of pain and improvement in function when compared to placebo and corticosteroids.3
Surgical treatment remains the most effective treatment for this condition. This would entail a trapeziectomy or excision arthroplasty of the base of thumb. In patients where there is associated STT joint arthritis, the procedure may be accompanied by a partial trapezoidectomy through the same incision. A study by Yeoman et al. in 2019 has concluded that there is a significant and sustained improvement in patient-reported function after simple trapeziectomy when patients were scored with QuickDASH and EuroQol questionnaires.4
The trapeziectomy may be combined with a ligament reconstruction and tendon interposition where a section of FCR (flexor carpi radialis) or APL (abductor pollicis longus) tendon is weaved into the excision arthroplasty after the trapeziectomy to suspend the thumb metacarpal in the void created. Occasionally a temporary k- wire is also inserted to provide further support.5,6 However the randomized double blind controlled study by Pace et al. comparing the 2 groups (trapeziectomy vs trapeziectomy and ligament reconstruction, interposition and k-wire) in 2009 concluded that the DASH scores and PEM (Patient Evaluation Measure) scores were reduced in both groups as did the key and tip thumb pinch but there was no significant difference between the 2 groups at either 3 or 12 months.7
In younger patients particularly manual workers a fusion of the CMC joint of the thumb may be considered as opposed to an excision. This is aimed at preserving grip strength. Although this procedure provides good pain relief, stability and length preservation, there is an associated decreased range of movement, inability to put hand down flat and a non-union rate of 12% and increased risk of predisposing adjacent joints to arthrosis.8
Prosthetic replacements of small joints are fraught with risks and complications and the same may be applied to arthroplasty of the thumb CMC joint and are thus not a popular choice of treatment. Some studies reveal a 40% risk of instability and dislocation.
Base of thumb arthritis is a common condition and can be debilitating to the function of the thumb and hand. Whilst most patients may be treated non-operatively, various different surgical procedures may be used with varying results.
SUMMARY
- Basal thumb arthritis is common and may be debilitating.
- Most cases may be treated conservatively.
- Injections have mixed results in patients.
- Trapeziectomy is the gold standard surgical procedure that gives long lasting pain relief and improved function.
REFERENCES
1. Higgenbotham C, Boyd A, Busch M, et al. Optimal management of thumb basal joint arthritis: challenges and solutions. Orthop Res Rev 2017; 9:93-99.
2. Malahias MA, Roumeliotis L, Nikolaou VS, et al. Platelet-Rich Plasma versus Corticosteroid Intra-Articular Injections for the Treatment of Trapeziometacarpal Arthritis: A Prospective Randomized Controlled Clinical Trial. Cartilage. First Published October 20, 2018. Epub ahead of print.
3. Papalia R, Diaz LA, Torre G, et al. Intrarticular injections of hyaluronic acid for trapezio-metacarpal osteoarthritis: a systematic review. J Biol Regul Homeost Agents 2017; 31(4 Suppl 2):45-53.
4. Yeoman TFM, Stone O, Jenkins PJ, et al. The long-term outcome of simple trapeziectomy. J Hand Surg Eur Vol 2019; 44(2):146-150.
5. Hutchinson DT, Sueoka S. A prospective, randomized trial of mobilization protocols following ligament reconstruction and tendon interposition. J Bone Joint Surg Am 2018; 100(15):1275-1280.
6. Reissner L, Marks M. Comparison of clinical outcome with radiological findings after trapiezectomy with ligament reconstruction and tendon interposition. J Hand Surg Eur Vol 2016; 41(3):335-9
7. Pace A, Davis T. Trapeziectomy for trapeziometacarpal joint osteoarthritis: is ligament reconstruction and temporary stabilization of the pseudoarthroisis with a kirschner wire important? J Hand Surg Eur Vol 2009; 34(3):312-21.
8. Zhang X., Wang T. Minimally invasive thumb carpometacarpal joint arthrodesis with headless screws and arthroscopic assistance. J Hand Surg Am 2015; 40(1):152-8.

