Vascular Surgery The Importance of Multidisciplinary Care in Diabetic Foot Amputations
Gloria Montebello & Prof. Kevin Cassar
Abstract
In Malta, 10% of the population over 18 years of age is estimated to be living with diabetes. This chronic condition can lead to complications which heavily impact our patients’ quality of life. In this case study, complications such as peripheral artery disease which can lead to ulceration and limb amputations are discussed. Providing care in an interprofessional team allows the sharing of best practice and expertise in order to achieve optimal results and ultimately save limbs.
Key Words
Diabetes, Diabetic foot, Amputation, Skin graft, Multidisciplinary care
A 55-year-old Maltese male patient who was diagnosed with DM in 2016 after developing chronic kidney disease 5 years before is now in end stage renal failure (CKD stage V) and is being managed with haemodialysis through a left radiocephalic fistula. The patient has a family history of diabetes in his family. He is a non-smoker and he is a social drinker. Other comorbidities include diabetic nephropathy, controlled hypertension, morbid obesity and hyperlipidaemia, all of which are being treated.
In 2019, the patient was referred to vascular surgery as he was approaching end stage renal failure. A left radiocephalic fistula at the distal forearm was fashioned. All arteries including the radial and ulnar were heavily calcified but the waveforms in both arteries at the wrist were triphasic. On needling, the venous pressures in the fistula were elevated. Left upper limb fistulography and central venography revealed a left subclavian vein stenosis that was successfully angioplastied.
In January 2021, he complained of a heavy, painful left foot with restricted movements. The second toe was dusky, all toes felt cold and he noted pus discharging from the 2nd toe. He was hospitalised by the vascular surgery team, for investigation and treatment. On assessment significant peripheral arterial disease was diagnosed with absent peripheral pulses and monophasic continuous waveforms at the ankles. Emergency transmetatarsal amputation of the left foot, and left superficial femoral, proximal posterior tibial and anterior tibial artery angioplasty was performed.
The gross diabetic foot infection was treated with IV 4g/0.5g piperacillin/tazobactam every 12 hours and teicoplanin IV 200mg daily. Bone cultures grew Morganella morganii which required IV antibiotic treatment for at least 6 weeks and a peripherally inserted ventral venous catheter (PICC line) was inserted in his right arm. The selection of antibiotic treatment was based on advice received from the microbiology team.
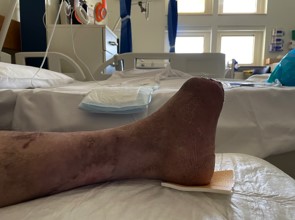
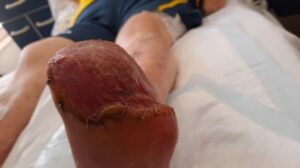
The transmetatarsal amputation site was treated with negative pressure treatment and after adequate granulation of the amputated site was achieved, a split skin graft was applied by the plastic surgery team to achieve skin cover.
Podiatric assessment and appropriate education about footcare were provided. Review by the orthotist was performed and he was measured for provision of footwear in an effort to prevent new ulceration. Daily sessions with the physiotherapy team were held to ensure that the patient retained good muscle tone and was able to bear weight safely. Blood glucose and blood pressure control was managed by the diabetologists. The tissue viability team reviewed the patient regularly and provided negative pressure treatment and dressed the surgical wounds appropriately.
The skin graft was healthy and complete skin cover of the amputated foot was obtained. Discharge from hospital was successfully planned with appropriate social support, close monitoring by the community podiatrists and regular physician review with regard to diabetes and blood pressure control. He will continue to be dialysed at the renal unit and his renal failure managed by the renal physicians.
Diabetic ulcers are a common cause of lower extremity amputation. Up to 25% of patients with DM will develop diabetic foot ulcers. It is reported that more than 50% of DM patients are unaware of the disease (as classified by the WHO).1 Common risk factors for amputation include diabetic neuropathy, structural foot deformity and peripheral arterial occlusive disease.2
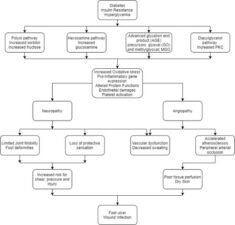
The pathophysiology of the diabetic foot is characterised by hyperglycaemia which drives neuropathy and vascular foot changes and can cause diabetic foot ulcers. Hyperglycaemia inhibits the production of nitric oxide (NO) by limiting endothelial NO synthase activation which can lead to superoxide formation. Enzymatically, superoxide is converted to hydrogen peroxide by superoxide dismutase. The superoxide anion binds to NO to produce peroxynitrite which limits the availability of a potent endothelium-derived vasodilator.
This disruption in endothelial function affects vasoconstriction, and causes platelet aggregation, abnormal intimal growth, inflammation and atherothrombosis formation. Atherogenesis may form due to the vessel wall characteristics with the interaction of inflammatory cytokines following glycoxidation and lipoxidation of vascular wall structural proteins. This atherogenesis of small vessels that supply peripheral nerves contribute to neuropathy.3
Vascular disease is the result of micro and macrovascular disease. The inflammatory response in the microcirculation leads to thickening of capillary basement membranes with arteriolar hyalinization. This comprises the normal transfer of nutrients and activated leukocytes between the capillary lumen and the interstitium. The inelasticity of capillary walls leaves a limited capacity for vasodilation in response to local injury and leads to functional ischaemia.4
Figure 1: Pathophysiology of diabetic foot ulcers.1
The patient’s main concerns were related to his mobility as he had recently lost his job due to the COVID-19 pandemic that contributed to his anxiety and affected his wellbeing. The patient was compliant to physiotherapy with balance exercises since his centre of gravity was altered. Factors that may delay wound healing include respiratory problems, immobility, diabetes, anti-coagulant therapy and any co-existent wound infection. Since the patient was allergic to penicillin, he was given teicoplanin.
The patient also received dietary advice to improve his blood glucose control and weight. Through social services, the patient was installing a stair lift in his home.
Multidisciplinary care is essential in the management of the diabetic foot. Routine foot examination to identify high-risk feet is part of all international recommendations for the care of patients with diabetes. Once an ulcer develops, continuous assessment of adequate perfusion, neurology and any potential infection is of utmost importance. Most ulcers require specialist care to prevent the deterioration and achieve resolution. A gap of interprofessional care may be due to busy schedules, lack of knowledge, lack of routine practice procedures and possible health care organizational barriers.5
This case report concluded that the patient did not recall any previous DM testing and there were no records of any pre-diabetes records. This window of opportunity for lifestyle change and early intervention for this patient have been missed. The management of diabetes and diabetic foot ulcers required interprofessional care from specialised nurses, vascular surgeons, diabetologists, podiatrists, orthotists, physiotherapists and occupational therapists. Moreover, the GP was also part of the team and should be a key player in the community to pick up pre-diabetic cases for early action and referral. Such a team-based framework is essential within our healthcare system in order to utilise best expertise to achieve optimal results and save limbs and function.

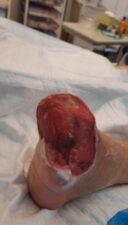
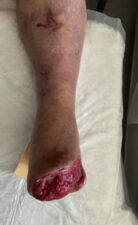
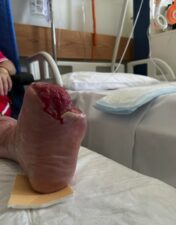
Figure 2: Wound assessment tool of the left foot.
References
1. Alavi A, Sanjari M, Haghdoost A, et al. Common foot examination features of 247 Iranian patients with diabetes. Int Wound J 2009;6(2):117-22.
2. Armstrong DG, Lavery LA. Diabetic foot ulcers: prevention, diagnosis and classification. Am Fam Physician 1998;57(6):1325-32, 1337-8.
3. Apelqvist J, Ragnarson-Tennvall G, Persson U, et al. Diabetic foot ulcers in a multidisciplinary setting. An economic analysis of primary healing and healing with amputation. J Intern Med 1994;235:463-71.
4. Eskelinen E, Lepantalo M, Hietala EM, et al. Lower limb amputations in Southern Finland in 2000 and trends up to 2001. Eur J Vasc Endovasc Surg 2004;27:193-200.
5. Boulton AJ, Armstrong DG, Albert SF, et al. Comprehensive foot examination and risk assessment: a report of the task force of the foot care interest group of the American Diabetes Association, with endorsement by the American Association of Clinical Endocrinologists. Diabetes Care 2008;31:1679-85.