Invertebrates in the medical service of man: Part 2 – The Insect Surgeons
Charles Savona-Ventura MD DScMed FRCOG AccrCOG MRCPI
Professor of Obstetrics & Gynaecology
Faculty of Medicine & Surgery, University of Malta
Invertebrates in the medical service of man:
Part 2 – The Insect Surgeons
- Savona-Ventura
MD, DScMed, AccCOG, FRCOG, MRCPI, CLJ, OMLJ
The invertebrates have generally been regarded as direct or indirect harbingers of disease conditions. Some species throughout history have however been used in lieu of surgical procedures. The example par excellence is the leech which was introduced in medical practice to perform venesection aimed at restoring the body humours envisaged by the Galenic theory of disease. These invertebrate surgeons were considered as a more gentle method for the procedure. Their use for venesection has slowly decreased in the latter part of the twentieth century, but the use of these animals has been resurrected in surgical practice for the biotherapeutic properties of their secretions [1]. Beside the Medicinal leeches, other insect species have been used as surgical assistants.
Phylum ANTROPODA; Class: Insecta;
Order: Diptera; Family: Calliphoridae
Bluebottle Fly – Calliphora vicina [Maltese – Zarzura]
Greenbottle Fly – Lucilia sericata [Maltese – Dehbija tal-Hmieg]
The primitive, carrion-breeding habit of the blowflies has been known and recorded for centuries. A very early reference can be found in the Hortus Sanitatus published at Mainz in 1491. The use of maggots to clean suppurating wounds was graphically demonstrated during the film “Gladiator” when the protagonist played by Russell Crowe was healed of his battle wounds through the use of maggots. It was however at the turn of the 19th century that the beneficial role of maggots was noted. Napoleon’s Surgeon in Chief, Baron Dominic Larrey reported that when maggots developed in battle injuries, they prevented the development of infection and accelerated healing. These insects, so far from being injurious to their wounds, promoted rather their cicatrization by cutting short the process of nature and causing the separation of cellular eschars which they devoured. These larvae are indeed greedy only after putrefying substances and never touched the parts endowed with life. There is no evidence, however, that Larrey deliberately introduced maggots into his patients’ wounds. Similarly, during the American Civil War, a Confederate medical officer Joseph Jones noted the beneficial effects of wound myiasis commenting that I have frequently seen neglected wounds filled with maggots, as far as my experience extends, these worms only destroy dead tissues, and do not injure specifically the well parts. I have heard surgeons affirm that a gangrenous wound which has been thoroughly cleansed by maggots heals more rapidly than if it had been left to itself. During that same conflict, the Confederate surgeon J. Zacharias may have been the first western physician to intentionally introduce maggots into wounds for the purpose of debriding the wound writing that During my service in the hospital in Danville, Virginia, I first used maggots to remove the decayed tissue in hospital gangrene and with eminent satisfaction. In a single day would clean a wound much better than any agents we had at our command…. I am sure I saved many lives by their use, escaped septicaemia, and had rapid recoveries‘.
The thought of intentionally introducing wriggling worms in gangrenous wounds rather than opt for a clean surgical debridement brings visions of medieval horror to doctors trained in a modern sterile hospital environment. Few of the doctors practicing in Malta today have experienced the surgical capabilities of fly maggots. I do however recollect one case of a maggot-performed amputation during the late 1970s. This occurred in a rather neglected geriatric female patient who had been admitted to the surgical ward with gangrene of the terminal part of one foot. When her home dressings were removed, the nurses were shocked to see a mass of wriggling maggot within the dead tissue of the foot. The Consultant Surgeon shocked everyone by deciding to utilize the maggots as his assistants rather than undertake surgical debridement in a medically-unstable individual. Within a few days the dead tissue had been completely removed by the insects and the dead bone remnants fell off, leaving a clean “surgical” healed plane. The patient recovered this event enabling discharge into a residential home.
The real founder of modern maggot therapy or wound myiasis was William Baer (1872-1931), Clinical Professor of Orthopaedic Surgery at the Johns Hopkins School of Medicine in Maryland. He first experienced the therapeutic potentials of maggot surgeons during the First World War. In 1928, he set out to experiment with the use of maggots in the treatment of intractable osteomyelitis in children. Repeated successes encouraged him to use the technique more widely, until several of his patients developed tetanus. In response to this complication, Baer set out to develop a suitable sterilizing process of the larvae and the eggs. Other workers enthusiastically took up this work and in the absence of any equally effective alternative for the treatment of osteomyelitis or infected soft tissue injuries, the use of maggots spread quickly during the 1930’s. These developments however coincided with the development of the antibiotic era which gave an effective medical therapeutic option. By the mid-1940s, the enthusiasm for maggot therapy virtually ceased and maggot therapy was used only sporadically.
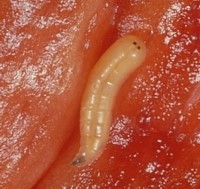
Blowfly maggot
A resurgence of interest in maggot therapy recurred in the late 1980s when Robert Sherman, an entomologist and physician in Los Angeles, noticed healthy infection-free tissue in a leg wound crawling with ‘worms’. He established an insectary in California to breed maggots for clinical use, and carried out the first controlled study showing that maggot therapy significantly increases the rate of healing of chronic pressure sores – at much lower cost than the usual regimen of repeated surgery and antibiotic treatments. The results of these preliminary investigations indicated that maggot therapy offered several advantages over other wound treatments currently employed. Maggot therapy has since grown in popularity and has met with success in Europe. It has recently been used in Germany, Hungary, Sweden, Belgium, and the Ukraine. In 1996, the International Biotherapy Society was founded to investigate and develop the use of living organisms, or their products, in tissue repair, and the first in a series of international conferences on maggot therapy and other similar topics also took place in that year [2,3].
Order: Hymenoptera; Family: Formicidae
Carpenter ant – Camponotus barbaricus [Maltese: Zokkrin]
Other members of the insect family have also been utilized in surgical practice since ancient times. Hindu writings dating to 1000 B.C. describe the use of ant mandables for closing incisions and wounds. The animal’s head is positioned so that the two parts of the mandable are situated on either side of the cut. They are then allowed to bite thus holding the wound shut like staple-stitches. The ants’ bodies are then pulled off, leaving only the heads and jaws locked in place until the wound heals. Ant stitching is reportedly still used by primitive societies in Brazil today. In Algeria and Turkey, beetle mandibles were the stitches of choice.

Carpenter ant
Order: Hymenoptera; Family: Apidae
Honey Bee – Apos mellifera [Maltese: Nahla ta’ l-Ghasel]
Honey has long been recognized as a sweetening food product and an “over-the-counter” medicine being utilized not only to make certain medicines palatable but also to sooth chest infections. It has also found use as a wound dressing, this medicinal function being described by the ancient Egyptians. Its role in controlling bacterial invasion and growth is based on its low pH value of 3.9, its hyperosmolarity, and the presence of INHIBINE or glucose oxidase which liberates peroxide acting as a strong antibacterial agent. Apitherapy, i.e. the medical use of honeybee products, is also gaining momentum. Anecdotal claims from the beekeeping community have suggested that bee-venom has a therapeutic value for joint inflammatory conditions. Bee-venom can be injected artificially via a syringe or simply by allowing live bees do the stinging. Bee-venom contains dozens of active chemical substances; some of which are known to have analgesic and anti-inflammatory properties. Bee-venom has been said to be useful for the management of migraine headaches and chronic pain. Bee-stings have also been reported to ease the symptoms of arthritis, bursitis, and rheumatism. The sting regimen for arthritis includes several stings per treatment performed two to three times per week for a period of up to three months.
Honey Bees

References
- Savona-Ventura, C. Invertebrates in the medical service of man: Part 1 – The Biotherapeutic Worms. Synapse, 2006
- Shinkman R.R. Worms and squirms. Maggots, leeches are making a comeback in modern medicine. Modern Healthcare, 2000, 30(43):p.54-55
- Maggot therapy: Website created by R.A. Sherman, January 1996, http://www.ucihs.uci.edu/com/pathology/sherman/cases.htm [accessed March 2006]

